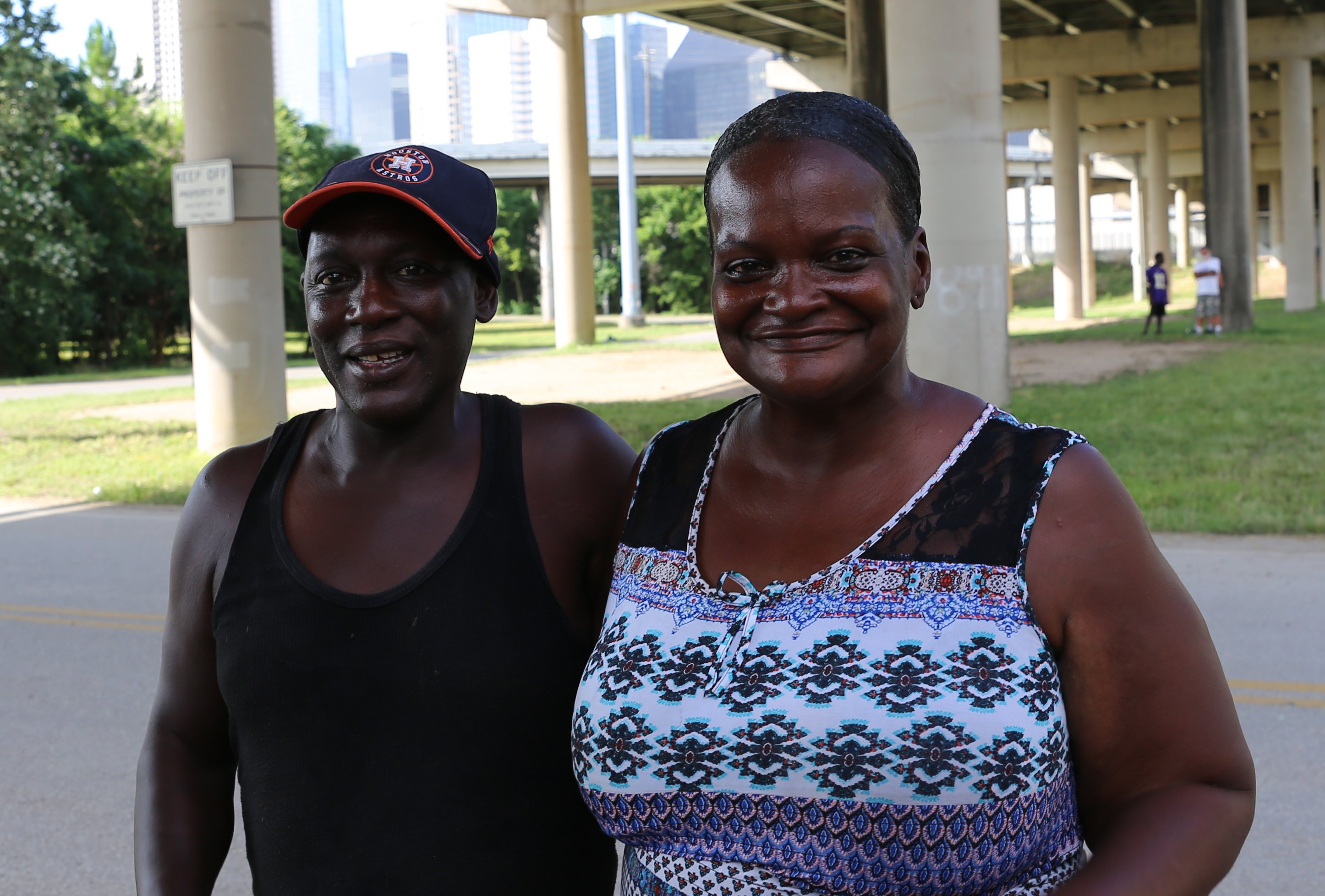Within the walls of your house, you have a roof to protect you from rain, a door to close to make you feel safe, and most importantly, a place to call home.
Yet many do not have this essential element from Maslow’s hierarchy of needs. In fact, Texas ranks fourth among states with the largest number of homeless individuals. Each night, more than 4,000 people in the Greater Houston area sleep without permanent housing—39% of those are unsheltered living under bridges or in tents.
While this number has ebbed and flowed over the decades, many remain chronically homeless, slipping through the holes of a tattered safety net of services and becoming high utilizers of health care.
Through a $2.5 million grant from the Substance Abuse and Mental Health Services Administration of the United States Department of Health and Human Services, Jane Hamilton, PhD, is leading an effort at UTHealth to combat behavioral disorders and homelessness.
Many chronically homeless individuals have struggled with mental illness all their lives, crippled by limited resources that leave them unsheltered. Hamilton says their primary diagnosis usually falls into one of four categories: schizophrenia, post-traumatic stress disorder, major depression, or bipolar disorder.
“There is a lot of stigma that makes them harder to house,” explains Hamilton. “It also takes a higher level of functioning to be in a shelter.”
Amplifying the impact of their disorder, unsheltered individuals are reluctant to take a medication that changes the way they feel. “They tell me that they don’t have a door, a place to be safe,” explains Hamilton. “So they worry about taking something that makes them feel a little different.”
Over the past 30 years, the percentage of adults over 50 years old in the homeless population increased from 11% to approximately 50%, revealing a problem compounded by time.
“I was driving around downtown Houston one evening when I saw all these people with white hair sleeping under a warehouse overhang,” remembers Hamilton. Often, family members who were once caring for them have died, leaving behind someone with medical comorbidities who is incapable of self-care.
On Jan. 18, 2019, Hamilton’s team added evidence-based mental health counseling and social services at The Beacon to improve patient access to and integration with primary care services provided by Healthcare for the Homeless. Within the first four months, her team enrolled 82 patients of the 500 the five-year grant is designed to treat. Eligible individuals with behavioral health needs are enrolled in a continuum of services, including evidence-based therapy and social services to assist patients with all needed benefits including Social Security Disability and to link patients with primary care, housing, and supported employment services.
Ninety percent of the patients her team treats have reported experiencing trauma. “Because the therapy offered in the program is trauma-focused, it is well-received by the patients,” she says. “They haven’t had access to this type of therapy in the past, and many even complete their in-between-session homework.”
But the integration of services doesn’t stop there. A common barrier for services is not having a government-issued ID. Many patients in the study grew up in the foster care system and moved around a lot, sometimes losing their ID card in the process.
“I had one patient who was born in Maine but entered the foster care system in California. She didn’t have her birth certificate to get an ID, so she’s been sleeping on the sidewalk for three years,” says Hamilton. “Our team helped her get her birth certificate, and she has received 35 therapy sessions in five months to address past trauma.”
Housing assessments must be conducted every 90 days for individuals to maintain eligibility for permanent supportive housing, which is a primary outcome of Hamilton’s work. This requirement introduces another barrier. “If they don’t get their housing assessment done every 90 days, no one follows up,” says Hamilton. “So we hired a dedicated housing assessor and have become a partner with Houston Coalition for the Homeless, the organization managing Housing and Urban Development funds for our region.” As a result, Hamilton’s team helped 23 people gain housing in less than five months—many of whom had outdated housing assessments when they enrolled in the program.
“People actually cry once we start moving them into housing because they are so scared and so frustrated with their lives. They just can’t believe it’s finally happening,” says Hamilton.
Many feel like the system has failed them. But with helping hands and research to improve services, Hamilton’s team is building relationships— and trust—to change the trajectory.
“Chronic homelessness is a sad thing that just shouldn’t happen,” says Hamilton, “especially when they have mental disabilities and cannot navigate complex and fragmented systems. By reducing chronic homelessness, we are making a positive impact on the health care system and, most importantly, the individuals.”

As a public health researcher with a background in sexual health studies, Vanessa Schick, PhD, wanted to enhance the health of women experiencing homelessness who engage in sex work for socioeconomic reasons. She joined forces with J. Michael Wilkerson, PhD, to investigate the health needs of individuals engaged in sex work and other individuals who make up the community of truck stops throughout Texas. What she thought would be a one-time visit revealed the complexity of these women’s needs and quickly morphed into regular visits.
By immersing herself in the space, Schick and her team found that these women’s needs were much lower on Maslow’s hierarchy than expected. “Any efforts to promote sexually transmitted infection screening would have been meaningless without addressing the underlying issues: food, shelter, security,” Schick explains.
In one early interview, an older woman shared that she had a good night; she had slept in a friend’s tent. “When I probed further, she said everyone fights over tents, but she didn’t have a home—referring to a tent as a home,” says Schick, “Not only were they living in tents, but many were even without the minimal safety and security that a tent could provide.” That night, Schick bought tents to hand out the next visit.
As part of the investigation, Schick helps connect the limited number of services available to people experiencing homelessness outside of urban areas, which is further complicated by weak public transportation.
“Some days, it feels like a family gathering. People are supportive of one another and welcoming to us,” says Schick. “Other times, it feels dangerous. Some people would engage with me as though I was working at the truck stops. It gave me the tiniest bit of insight into the disrespect that these women encounter daily.”
As the truck stop story lingers, Schick continues to bring her public health toolbox to help this disenfranchised population. “What’s complicated about the truck stop narrative is there aren’t good and bad guys,” she says. “There are just a lot of people trying to get by.”